The 1st International Conference on Safety and Public Health
More infoThis study aimed to find out the opportunity of artificial intelligence (AI) and the risk in health service.
MethodA comprehensive literature search was collected from three databases (Web of Science, Google Scholar, and EBSCOhost) to identify articles studied Implementing AI in improving in health services. Two reviewers independently assessed the quality of studies using the Joanna Briggs Institute.
ResultsThe application will improve diagnostics, prevention, and treatment of patients, increasing cost efficiency and equality and equality in health services. For the challenge, there is no AI adoption in public sector, patients’ privacy, patient autonomy rights become problems in AI applications.
ConclusionsImplementation of AI is needed in the efficiency of health service management as well as making medical decisions. The challenge is facilitating early adoption and ongoing implementation in the health care system, and we consider some of the ethical problem lists faced by AI clinical application.
Artificial intelligence (AI) rapidly dominates the health service system. It removes the manual health system into automatic, in which humans conduct the routine works/tasks in medical practice to the management of patients and medical resources. The technical challenges of digitizing health services pose new problems when developers create artificial intelligence systems to carry out tasks.1
AI offers the potential for a huge improvement in patient care and a reduction in health care costs. The increasing population is expected to be able to encourage the demand for health services. The health service sector needs innovative solutions to find out how to be more effective and efficient without excessive expenditure.2 This is where technology comes in for the solutions. Rapid developments in technology, especially in the fields of AI and robotics, can assist the complement of the healthcare industry.
AI and robotics in health care using artificial intelligence develops quickly, especially for early detection and diagnostic application.3 Ai is becoming more powerful at the same time. It enables them to do what humans perform — often more efficiently, easily, and at reduced cost.
Some risks and challenges appear, including the risk of injury to patients from system errors, the risk of patient privacy in obtaining data and drawing conclusions from artificial intelligence, and more.4 The important thing for public health is that AI preventative care can assist people to stay healthy. For example, applications, the aim is to give better control over their health and welfare to consumers.
AI is highly needed for early detection and diagnostic. It is used in various ways to detect diseases such as cancer more accurately, reliably, and quickly. Simply put, it works by comparing data from some patients, including pictures of vast quantities of other patients’ data. The independent learning system detects association and suggests a diagnosis. For instance is Google's DeepMind Health Technology integrates machine learning with a neuroscience system to model the human brain using AI and provides diagnostic and decision-making support to healthcare professionals.5
This novel technology is used more efficiently in administrating medical care. The future of AI in health care is not fully optimistic because there are advantages in the process. Numerous questions arise whether AI can exercise doctors’ rights and obligations, protect privacy issues, and the applicable law is not fully prepared with this progress. The use of AI for the healthcare system in the world indicates that current regulations support it. It is proven that the rules in the development of technology and health technology products can be developed and applied for medical care.6 This study aimed to find out the opportunity of AI and the risk in health service.
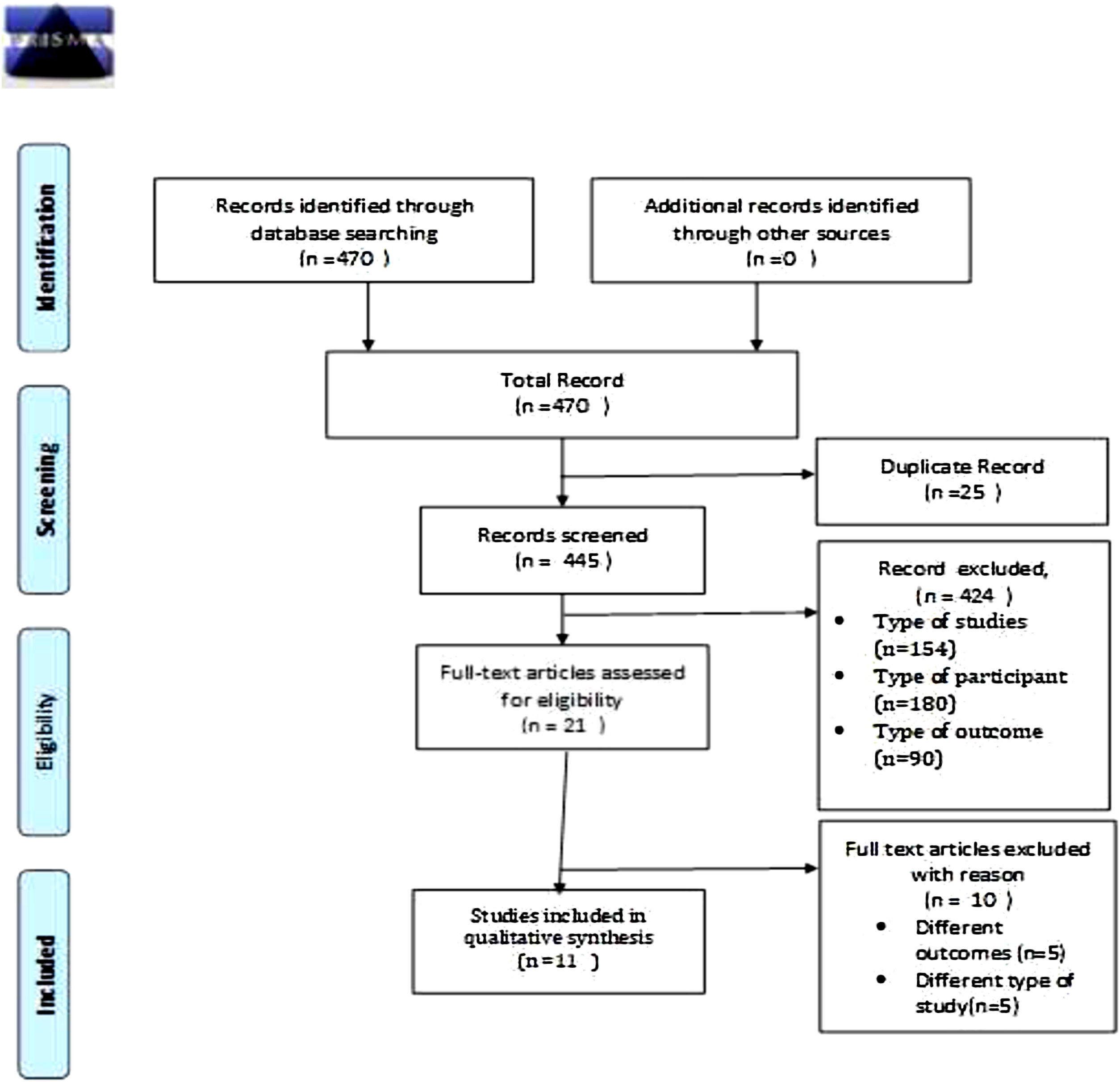
MethodsThe methodology used in arranging this literature study was depicted through the flowchart (Fig. 1).
For a short explanation, PRISMA flowchart7 uses the methodology of writing a literature review using PICO. It is the framework used to develop literature search strategies as well as using Quantitative Research methods. The search strategy was as follows: Data were collected from 3 databases such as Web of Science, Google Scholar, and EBSCOhost with the combination of word search of Implementing Artificial Intelligence in Improving Health care in Hospitals or Primary Health care, Artificial Intelligence in Health Services. Opening a Science Direct website contains paper-journals. The papers sought were from 2010 to 2020 in English, and only original articles were selected for analysis. Two hundred nine papers were obtained in 10 years period. Of the 209 papers, some more specific papers were selected to obtain the appropriate paper. The papers selected were those that have the closest title with the aim of writing this literature review. The number of the chosen papers were 11 papers. Furthermore, the authors read the abstracts and conclusions of the selected papers and analyzed the papers.
ResultsThe research type of this paper includes five journals1,2,8,9 about applying AI, three journals about challenges and benefits of AI1,10,11 and three journals about problems in the application of AI in health services.3,8,9
The application of artificial intelligence in health serviceIn this era, the role of technology is very important. Technology plays a role and aims to ease human work and to make it more efficient. Besides, in the health sector, technology plays an important role in minimizing errors caused by human negligence. For instance, if there is no role of technology in surgical operations performed by doctors, the operation can be dangerous and lead to failure. In other words, AI is a simulation of human-made intelligence in machines programmed to think like humans. AI will improve patient diagnostics, prevention, and therapy and to improve clinical decision-making.12
Challenges and benefits of artificial intelligenceThe application of AI in health service can cause challenges or benefits. The application of technology in healthcare has clear benefits, such as improving patient management choices and outcomes, as well as potential secondary benefits such as fewer referrals, reducing costs, and saving time. It can also assist health facilities in rural areas and promote recruitment and retention in rural areas. Ultimately, this can contribute to a more equitable system of global health care,1 the challenges are facilitating early adoption, and sustainable implementation in the health system, lack of consideration for the user's perspective, and technology cannot be used optimally but the need for adoption of AI in the public health sector. In the public health system, the adoption of AI offers a blueprint for the flow of research that focuses on different aspects of the adoption of AI in the public system.10
The problem in application of artificial intelligence in health serviceThe efficacy of AI in improving the aspect of health service administration has proved. AI will likely be included in routine clinical care soon. However, concerns regarding the ethical and laws implications of introducing AI in healthcare have been expressed. These concerns include the risk of bias, lack of clarity for some AI algorithms, privacy issues for data used for AI model training, and security issues and AI implementation responsibilities in clinical settings. There are some of the ethical problems faced by AI clinical applications. They are safety, efficacy, privacy, information and consent, the right to decide, “the right to try,” the costs, and access.13
DiscussionThe applications of artificial intelligence in health serviceThe application of AI is the right way for the development in the health sector, especially Health Service. However, there will be an impact on AI application, such as a system error and ethical issues and regulations.
EquityIn the sense of health, moderate images, text from patient reports on medical conditions, diagnosis and care, and cost reimbursement codes may be included, but not limited only. Inaccurate and under-representative training data sets for AI models, as discussed previously, can cause bias, misleading predictions, adverse events, and even large-scale discrimination.8
TransparencyWhile the deep learning model's performance in the analysis of medical image and clinical risk prediction has been highly promising, this model is also difficult to interpret and explain. The difficulty raises certain problems in the world of medicine, where transparency and the ability to explain clinical decisions are very important.8
TrustPhysicians need to consider the cause and effect of medical problems, and the techniques and models used to help the decision-making process of the doctor, in the case of AI. Besides the clarification issues discussed in the previous section, the potential for AI applications’ Autonomous functions and the possible susceptibility to accidental or malicious tampering of these applications to produce unsafe results may present a major obstacle for doctors to recognize AI in their medical practice.8
AccountabilityAccountability is the fourth and the last part of our proposal for governance. This begins with the development of the AI model and extends to the extent that the model is used in clinical care and, ultimately, retirement. This scope includes many players, including developers of software, government officials, health care, medical practitioners, and advocacy for patients groups.14
The use of AI in health service is not only for increasing clinical capacity but also for administrative capacity. AI can be conducted with telemedicine for distributing health-related services and information by utilizing communication technology, assuming the implementation of telemedicine will greatly affect the business model in hospitals.15
Challenge and benefit of artificial intelligenceThe development of the health sector currently does not grow maximally. A promising field of AI application is the public health service. Although implementation is slow, its use continues to increase because of the potential cost savings at the core of health care delivery, AI will replace face-to-face experiences. In many respects, the use of AI has been generally considered possible to redesign the health sector.
The virtual branch concerns the center of AI, including the study of in-depth knowledge processing for health management systems, electronic health records, and the active supervision of doctors in their medical decisions.16 The use of AI systems to assist doctors in patient diagnosis, in particular, has recently received research attention. In the future, this AI can detect various other diseases, when updated with more sophisticated technology and equipped with more complete data.
The technology in healthcare has clear benefits, such as improving patient management choices and outcomes and potential secondary benefits such as fewer referrals, reducing costs, and saving time. This can also help reduce professional isolation and promote recruitment and retention in rural areas.17 In turn, this can contribute to a more equitable system of global health care in poor-resource settings in high- and low-income countries.
Problems in the application of artificial intelligence in health service1) Data biasTraining of the AI model needs a big scale of input regarding health data or others. Such bias may occur when the data used for training does not reflect the target population and when insufficient or incomplete data is used to train AI models, there may be unrepresentative data due, for example, to social discrimination (lack access to services health) and relatively small samples (for example, minority groups).18
2) PersonalHealth service data are the most sensitive information that can be owned by an individual about another. In health care, respecting the privacy of an individual is a vital ethical principle because privacy is bound by patient autonomy or self-government, personal identity and well-being.8 Thus, it is ethically important to respect patient confidentiality and ensure adequate processes for obtaining correct consent.
3) The principle of ethical double effectsConsidering that science is a backsword, certain findings ultimately cause damage. This is very suitable for special borders in AI. Therefore, the principle of double effect ethics must be carefully considered in applying AI, for example, stem cell research and gene editing.9
4) Problem of ethic related to research and biomedical medicineAs all new scientific techniques, biomedical ethical principles must be obeyed by AI in healthcare applications. They are autonomy, benefit, non-crime, and justice. They are manifested as consent, privacy, and safety, voluntary participation, autonomous decision making, etc., which should be considered and practiced in any implementation.9
ConclusionsThe application of AI is needed in health services, especially in the management of health services, to make medical decisions, especially predictive analysis, in diagnosing and treating patients. The challenges are facilitating early adoption, sustainable implementation in the health system, lack of consideration for the user's perspective, Technology is not optimally used, but is necessary for the adoption of AI in the public health sector. Some of the ethical problem lists faced by AI clinical application, there are safety, efficacy, privacy, information and consent, the right to decide, “the right to try,” the costs and access.
AcknowledgmentsThis research was supported/partially by Universitas Muhammadiyah Kalimantan Timur. We are grateful to our colleagues who provided expertise that greatly assisted the research, although they may not agree with all of the interpretations provided in this paper.
Conflicts of interestThe authors declare that they have no conflict of interest.
Peer-review under responsibility of the scientific committee of the 1st International Conference on Safety and Public Health (ICOS-PH 2020). Full-text and the content of it is under responsibility of authors of the article.