This study explores nurses’ perspectives on how the financial crisis and austerity measures introduced in the Spanish Health System affected their ability to provide care in these new circumstances
MethodCross-sectional observational study. In 2013, during an international annual congress in Spain, 123 nurses out of a total of 350 attendees completed a 14-item open-ended response questionnaire to examine the perceived impact of the financial crisis and austerity measures on quality of services and their experiences at work.
Results84% of the sample were women and the mean age of the respondents was 40 (standard deviation: 11.13). Seventy-seven percent of the nurses reported austerity measures introduced in their workplace. The nurses voiced strong disagreement with austerity measures (86%), due to the negative repercussions on nurses’ working conditions (47%), a decrease in human resources (37%), negative effects such as work overload (37%); a perceived deterioration in the quality of healthcare (77%) and pharmaceutical services (86%); and worsening conditions in access to health services by vulnerable populations (43%), leading to ethical dilemmas in clinical practice (26%).
ConclusionThis study showed that nurses participating in this study overwhelmingly opposed austerity measures imposed on the National Health System as a response to the financial crisis, which had a negative effect both on nurses’ working conditions and on the quality of health services. Institutional measures to improve recruitment and retention of nurses including policies for preventing stress and burnout, a decrease of patient-nurse ratio, and greater work stability should be considered.
Explorar la perspectiva de las enfermeras sobre cómo la crisis financiera y las medidas de austeridad en el Sistema Nacional de Salud afectan al cuidado que prestan en España.
MétodoEstudio observacional transversal. Durante un congreso internacional anual celebrado en España en 2013, 123 enfermeras de un total de 350 asistentes completaron un cuestionario compuesto por 14 ítems de respuesta abierta, para examinar las consecuencias percibidas de la crisis financiera y las medidas de austeridad en la provisión de los cuidados.
ResultadosEl 84% de la muestra eran mujeres con una media de edad de 40 años (desviación estándar: 11,13). El 77% reportó medidas de austeridad en su lugar de trabajo y el 86% mostró un fuerte desacuerdo con las medidas de austeridad debido al descenso en los recursos humanos (37%), la sobrecarga de trabajo (37%) y el deterioro de sus condiciones de trabajo (47%), de la calidad de los servicios de salud (77%) y farmacéuticos (86%), y del acceso a los servicios de salud de las poblaciones vulnerables (43%), que lleva a dilemas éticos en la práctica clínica (26%).
ConclusiónLas enfermeras que participaron en este estudio se oponían de manera abrumadora a las medidas de austeridad impuestas al Sistema Nacional de Salud como respuesta a la crisis financiera, que han tenido efecto negativo tanto en sus condiciones de trabajo como en la calidad de los servicios. Se necesitan medidas institucionales para mejorar el reclutamiento y la retención de enfermeras, incluidas políticas para prevenir el estrés y el agotamiento, una disminución de la relación paciente-enfermera y una mayor estabilidad laboral.
The global financial crisis beginning in 2007 resulted in the introduction of austerity measures in most of the affected countries.1 Spain was one of the European countries hardest hit by the economic crisis,2,3 with austerity policies in public expenditure being introduced in 2010 affecting the resources available in Spanish National Health System (NHS).3,4 Austerity measures resulted in NHS personnel/public employees’ wage freezing and salary reductions (up to 5%), increasing working hours for existing staff, and a staff recruitment freeze.4,5 Between 2009 and 2014, staff expenditure of de NHS decreased from 31.223.857 to 27.766.868 euros, with a strong reduction on primary health care expenditure (from 8.366.581 to 6.997.544 euros) compared to hospital care (from 20.451.063 to 18.422.814 euros).6
Reductions on the national and regional budgets were applied from 2009 to 2016. Health expenditure in Spain followed an upward trend until 2009 when the trend reserved and health expenditure decreased each year until 2016.7 As a result of these consecutive decreases in funding, between 2009 and 2015, government expenditure on health decreased 5.3%.8 In April 2012, The “Royal Decree-Law 16/2012, of urgent measures to ensure the Sustainability of the National Health System and to improve the Quality and Security of its Provisions” (hereafter referred to as: RDL/2012) was approved. In this law, measures were introduced with the aim of undertaking a structural reform and achieving a more efficient healthcare system, although health expenditure in Spain is below the average within the European Union and its growth is 1.4% lower than the combined average of OECD countries.4,5,8 In 2012, health spending was reduced by 8% in comparison to the previous year,9,10,11 by reducing the free health coverage portfolio, establishing and increasing co-payments for certain benefits (e.g., ambulances, hospitalizations, and pharmaceutical assistance)and introducing restrictions to health care services.5,12,13 With this legislation, only the insured and their beneficiaries were entitled to full assistance, and people who are considered uninsured had restricted access to primary health care and specialized care; they could only access emergency services in cases of severe illness or in the event of an accident, and only women in pre-natal, natal and post-natal situations, and people under 18 years of age could have general access to health care services.
Previous studies have examined the impact of the financial crisis on the health of the population and the impact of austerity measures on access to the health services and to a lesser extent, on how these affect the daily work of health professionals, mainly physicians.2,12,14–16 However, little is known about how these legislative measures affected nurses’ daily work. Nurses account for 54.20% of the total health care professionals in Spain, they are the front-line health care providers and an important source of information to patients.17 The aim of this study is to ascertain the perspectives of nursing professionals on how the financial crisis and austerity measures affected their ability to provide care in such new circumstances.
MethodDesignThis is a cross-sectional observational study based on data from a questionnaire with open-ended questions.
ParticipantsThe study population included the nurses attending the annual International Congress organized by Investen-Institute of Health Carlos III (Ministry of Economy and Competitiveness) that took place November 2013 in Lleida (Spain). This annual congress was chosen for the study because it is a place where Spanish nurses meet to exchange knowledge and results from their research on health services.
Sample sizeThis study was carried out with a nonprobability convenience sample: 350 nurses attending the congress’ closing session. The cross-sectional survey is representative of nurses attending the congress. The only inclusion criteria were being registered for the congress and working in Spain. The final sample consisted of 123 people who answered the questionnaire.
Data collectionNurses were invited to participate in a survey by two members of the research team during the meeting. An anonymous, self-administered questionnaire was designed and handed out during the congress’ plenary session. This questionnaire consisted of 27 questions organized into 18 main questions and 9 multi-choice auxiliary questions, under three sections: 5 closed-ended dichotomous questions (yes/no) on socio-demographic data, professional background and the expertise of the respondents, 13 closed-ended main questions, and 9 auxiliary open-ended questions on the impact of the crisis and the austerity measures on health care (see online Appendix). The selection of questions was based on a literature review focusing on the impact of austerity measures on several areas18 and previous qualitative research conducted by some of the authors in this study.19,20
Ethical considerationsPrior to the distribution of the questionnaire, all participants were informed about the main objectives of the study. The questionnaire had an explanation about the voluntary nature of participation and the anonymity and confidentiality of information treatment. The study had previously received the approval from the University of Lleida board of ethics.
Data analysisData were analysed with the statistical software SPSS v.22 using descriptive statistics. Socio-demographic data were described using univariate statistical parameters. Confidence intervals of 95% were also calculated. Frequencies of the answers provided, absolute percentages, and the existing relation between the variables were calculated. The main variables used in the analyses had a maximum of 0.81% missing values. The tables presented in the Results section correspond to complementary questions.
If a participant gave more than one answer, all of them were registered. The answers to the open-ended questions of the questionnaire were categorized and reduced to new variables. The questionnaire was designed and administrated in Spanish. Categorization of responses were conducted in Spanish. The questionnaire and findings were later translated for publication purposes.
Results35.1% of nurses attending the Congress answered the questionnaire. Out of all 123 surveys included in the final analysis 122 had all 14 main questions answered in full, and 85 had at least one or more unanswered auxiliary questions.
Description of socio-demographic characteristicsA high percentage of participants were women (84%) aged between 20 and 66 years with an average age of 40.65 years (standard deviation: 11.13). A total of 52% of participants worked in hospital care, 25.2% in primary health care, 11,7% in the Academia, 7,5% were unemployed and 1,7% work in long term care settings. 17.1% work in a rural environment and 82.9% do so in an urban environment. 57,7% worked in Catalonia, where the Congress was held, and the rest of them were based in 13 autonomous communities (10,6% Madrid, 7,3% Murcia, 6,5% Andalucía).
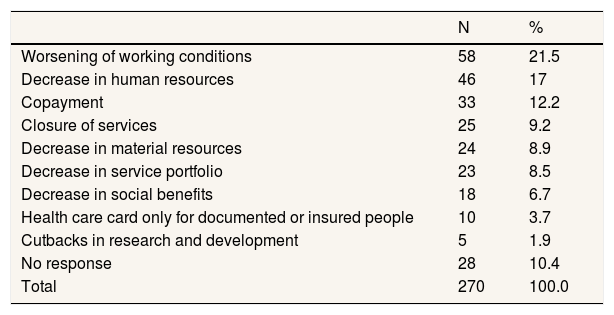
Nurses’ disagreement with austerity measuresA total of 77.2% of nurses identified austerity measures that have been applied to their workplace are affecting their everyday work. A total of 47% of nurses reported a worsening of their working conditions, 37% a decrease of human resources and 27% the existence of a pharmaceutical co-payment (Table 1).
Application of austerity measuresa.
| N | % | |
|---|---|---|
| Worsening of working conditions | 58 | 21.5 |
| Decrease in human resources | 46 | 17 |
| Copayment | 33 | 12.2 |
| Closure of services | 25 | 9.2 |
| Decrease in material resources | 24 | 8.9 |
| Decrease in service portfolio | 23 | 8.5 |
| Decrease in social benefits | 18 | 6.7 |
| Health care card only for documented or insured people | 10 | 3.7 |
| Cutbacks in research and development | 5 | 1.9 |
| No response | 28 | 10.4 |
| Total | 270 | 100.0 |
The majority of nurses (86%) disagreed with the introductions of austerity measures. Table 2 summarises the reasons for their disagreement, such as considering that austerity measures should be introduced in other areas, or that austerity measures harm the population and patients’ safety.
Reasons for rejection of austerity measures. Frequencies and absolute percentagesa.
| N | % | |
|---|---|---|
| Austerity measures should be introduced in other areas | 29 | 23.6 |
| Austerity measures harm the population and patients’ safety | 26 | 21.1 |
| Austerity measures are against the law and people's rights | 14 | 11.4 |
| Austerity measures foster social inequalities | 12 | 9.7 |
| Austerity measures harm health professionals | 6 | 4.9 |
| Other reasons (are not efficient in the long term, are not justified, nurses also feel affected as users) | 5 | 4.1 |
| No response (no rejection or no answer) | 31 | 25.2 |
| Total | 123 | 100 |
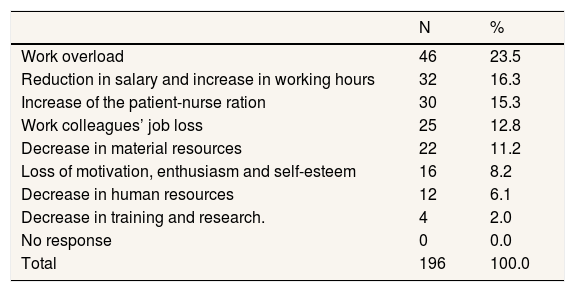
Regarding the specific consequences on nurses’ working conditions, all of them (100%) reported negative effects such as work overload (37.4%), the reduction of their salary, an increase in working hours (26%), and an increase in the patient-nurse ratio (24.4%) (Table 3).
Main problems of the population derived from the crisis. Frequencies and absolute percentagesa.
| N | % | |
|---|---|---|
| Increase in mental disorders (depression, anxiety and suicides) | 44 | 33.3 |
| Increase in social inequalities | 22 | 16.7 |
| Problems related with malnutrition | 22 | 16.7 |
| Chronic diseases (diabetes, obesity…) | 22 | 16.7 |
| Deterioration of living conditions | 16 | 12.1 |
| Fear of the population of losing access to the public health system | 14 | 10.6 |
| Increase on transmissible diseases | 13 | 9.8 |
| Problems derived from job/unemployment conditions | 10 | 7.6 |
| Decrease in hospital admissions | 4 | 3.0 |
| No response | 0 | 0.0 |
| Total | 132 | 100.0 |
A percentage of 26.8% had experienced a situation leading to an ethical dilemma regarding the care for patients with no health care card, restrictions to issue prescriptions, treatment and diagnostic tests, follow-up difficulties and poor treatment adherence from patients for not being able to afford medicines, early patient discharge, emotional impact for attending patients in precarious situations and professionals’ presenteeism.
Consequences of the austerity measures applied to the NHS on the population
A total of 79% of nurses considered that the financial crisis had affected their patients. Among the problems identified in their practice, 44% of nurses reported an increase in mental disorders such as depression, anxiety, and suicides (Table 4).
Consequences of the austerity measures on the nurses’ daily work. Frequencies and absolute percentagesa.
| N | % | |
|---|---|---|
| Work overload | 46 | 23.5 |
| Reduction in salary and increase in working hours | 32 | 16.3 |
| Increase of the patient-nurse ration | 30 | 15.3 |
| Work colleagues’ job loss | 25 | 12.8 |
| Decrease in material resources | 22 | 11.2 |
| Loss of motivation, enthusiasm and self-esteem | 16 | 8.2 |
| Decrease in human resources | 12 | 6.1 |
| Decrease in training and research. | 4 | 2.0 |
| No response | 0 | 0.0 |
| Total | 196 | 100.0 |
Of the participating nurses, 95 (77%) affirmed that austerity measures applied to the Health Services affected population health. Table 5 shows in more detail the main consequences the impact of the austerity measures on population health, such as decrease in quality of care and delay in service delivery (35%), increase in waiting lists (25%), and an unequal access to prevention programmes due to an increase in social inequalities (18%).
Main consequences of the austerity measures applied to the NHS on the population. Frequencies and absolute percentagesa.
| N | % | |
|---|---|---|
| Decrease in quality of care and delay in service delivery | 43 | 35 |
| Increase of waiting lists | 31 | 25.2 |
| Unequal access to prevention programmes due to the increase in social inequalities | 22 | 17.9 |
| Changes in the patient profile | 19 | 15.4 |
| No effect | 6 | 4.9 |
| Other consequences such as greater demand of A&E or lack of therapeutic adherence | 5 | 4 |
| Non response | 7 | 5.8 |
| Total | 123 | 100 |
Of those surveyed, 48.0% appreciated that based on their experience fewer patients currently accessed health care services. The main reasons for the decrease in accessing health care services identified by nurses were the cost of medicines; service and transport co-payment; waiting times; elderly patients having to care for relatives; lack of information about services; and work reasons (patients are denied permission to go to health centers or do not have health care coverage).
A high percentage of nurses (85%) believed that co-payment for medicines has had an effect on the most vulnerable population (pensioners, the unemployed, etc.). The main negative effects of co-payments were increased impoverishment and an increase in inequalities (47%). Only 9% of respondents agreed on the benefits of co-payment for medicines, of which 6% reported that it had resulted in a more responsible medicine consumption.
Effects on migrant populationThe effects of the financial crisis and austerity measures on migrant population include the change in access to health services and worsening of health conditions due to an increase in infectious diseases. A total of 43.1% nurses stated that there had been a decrease in access to health services by the migrant populations. Nurses explained this decrease as a result of migrants now accessing A&E services more often and only for acute pathologies (42%); migrants being unable to access services because they do not have a health card (40%); other access barriers (12%) caused by circumstances such as co-payments (4%) or the return to their country of origin (2%). In addition, 33% of nurses perceived an increase in infectious diseases among migrant population, of which 14.3% could be attributed to problems in accessing health services and treatment, 12.5% to worse living conditions and 4.9% to a decrease in health educational programmes.
No statistically significant differences were found between sex, age groups, rural or urban environment, autonomous region or labour group.
DiscussionThis research has highlighted nurses’ overall opposition to austerity measures imposed on the NHS as a response to the financial crisis. The main reasons reported include a perception that such health reforms were having negative consequences on nurses’ working conditions, the deterioration of the quality of health services, and that austerity measures were having a negative effect on the health of both nationals and migrants’ populations.
The implementation of the RDL/2012 during a time of deep economic crisis, brought about health staff reductions caused by the sudden reduction in employment offers, especially public recruitment, the main job generator among health care professions and nursing in particular.17,21 Potential long-term negative results, beyond the period of recession were evident in England, where decrease in NHS's human resources investment entailed a decrease in the nurse-patient ratio, work overload for nurses and a decrease in the quality of care, which had an impact in the health of the population.22–24
Nurses’ reported a decrease of patients in their practice, mainly due to the increase in waiting lists and delays. This could result on patients accessing private services to avoid long waiting times.2,4,25,26 Indeed, between mid-2009 and 2012, surgery waiting lists grew by 43% in number of patients, with an average increase in in waiting times from 63 days to 76 days (21%).27 Data from the Spanish Health Ministry shows that surgery waiting lists have gone slightly down from 614.101 to 592.175 during 2017, although unequally between Autonomous Regions28,29.
Nurses reported the precarization of their working conditions through salary reduction and increase in working hours, coinciding with official statistics.21 Precarious working conditions which nurses endured -manifested in the loss of job security, loss of social benefits, and night shift and weekend benefits, the increase in working hours, little time to devote to direct care, lack of job replacement following retirements, the increase in casual and temporary positions to the detriment of permanent positions, resulted in work overload and had a negative impact on the quality of care and on nurses’ own quality of life.5,30,31 The current situation can lead to an increase in the prevalence of burnout among nurses, whose figures ranged between 18% and 33% in 2013, while between 26.74% and 55% report emotional exhaustion.32
As a consequence of the global economic crisis, the organizational changes in the Spanish NHS, the reduction in public expenditure, and labour market reforms, more nurses than any other health professionals in Spain have migrated to work in other countries in search of better working conditions.33,34 Between 2010 and 2014 there was an increase in the migration of Spanish nurses, from 4580 to 9200 Spanish nurses working in other European countries, such as Great Britain and Germany33,35,36.
Creating and maintaining such a work environment to retain and support nurses is key in improving the quality of care and patient safety, so future measures ought to be considered. These include, among other, institutional measures to improve recruitment and retention of nurse; policies for preventing stress and burnout; ensuring a decrease of patient-nurse ratio; and promoting greater work stability.
Studies carried out in Spain based on primary health care services also showed that physicians’ perceptions were of disapproval of the austerity measures implemented in Spain to make the health system sustainable, considering them inappropriate and inefficient.14,15 A large number of health care professionals, with the support of their professional associations, unions, and the 15-M movement declared that they would refuse to stop giving care to foreign patients due to administrative irregularities, national agencies and scientific societies also seconded this rejection. As a consequence, constitutional challenges were filed to avoid complying with the restrictions of access for vulnerable groups in some Autonomous Regions.37 In 2018, new RDL 7/2018, of July 27, modifying the previous RDL/2012 and partially recovering the universal access to the NHS was implemented, so the effects of the changes introduced should be explored in the near future.
LimitationsThe limitations of this study include: 1) a relatively low rate of participation, 35.1%, although it is representative of the nurses attending the congress. In order to avoid social desirability bias, which the use of a self-administered questionnaire could lead to, answer-filling was anonymous; 2) the group that responded has no representativeness by sector of work; 3) due to the high percentage of nurses working in Catalonia in the sample, as it is a congress that was held in Catalonia, may have influenced the representativeness of these results at state level; and 4) no association were found in this study between nurses’ gender, working environments or autonomous regions, which his could be explained because data were collected a short time after the RD/2012 was implemented, and the low n of the rest of the 12 autonomous regions to which the participants belonged, where the RD was implemented unequally, did not allow a regional comparison to be made.
ConclusionOur findings suggest that participating nurses’ overwhelmingly opposed austerity measures imposed on the NHS as a response to the financial crisis. To our knowledge this is the first study exploring nurses’ perceptions on the effects of austerity measures on health care in Spain, only one year after these measures were introduced. The results of this study are especially relevant, as nurses are the NHS’ primary workforce and with the closest contact with patients.
The “Royal Decree-Law 16/2012, of urgent measures to ensure the Sustainability of the National Health System and to improve the Quality and Security of its Provisions” introduced measures with the aim of undertaking a structural reform and achieving a more efficient healthcare system.
What does this study add to the literature?This study shows strong disagreement with austerity measures among Spanish nurses, due to the negative repercussions on nurses’ working conditions and a perceived deterioration in the quality of health services as well as worsening conditions in the access to health services by vulnerable populations.
María Victoria Zunzunegui.
Transparency declarationThe corresponding author on behalf of the other authors guarantee the accuracy, transparency and honesty of the data and information contained in the study, that no relevant information has been omitted and that all discrepancies between authors have been adequately resolved and described.
Authorship contributionsFalta.
AcknowledgmentsWe thank all nurses who provided support and helped in the acquisition of data. The authors are also grateful to Roland Pastells, who provided support with the documentation.
FundingNone.
Conflicts of interestOne of the authors (EBV) belongs to the Gaceta Sanitaria editorial committee, but was not involved in the editorial process of the manuscript.